*AMPERNA® products are cosmetic only and not intended to treat, cure or prevent any disease or skin condition. Always consult a healthcare professional for medical advice.
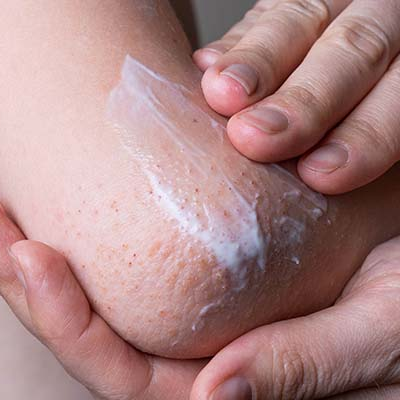
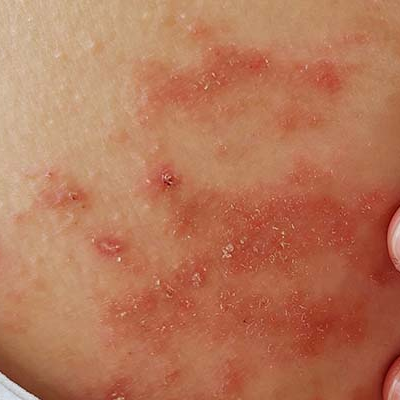
Eczema
Eczema often starts as an itchy, red patch on your elbows, neck or behind your knees, and boy does it drive you mad. It can really affect your quality of life, limiting your ability to do some of the things others take for granted and making you feel like hiding yourself away.
Australia has one of the highest incidences of eczema and unfortunately, it’s on the rise (Source: ABC.net.au).
‘I was born with eczema and have suffered on and off all of my life. It has been so bad that I was nearly hospitalised at one point. It’s very uncomfortable and at times all consuming.
My skin becomes itchy like it’s crawling, and very hot. Scratching feels so good, but also makes it a lot worse.
I have tried lots of things with varying and usually minimal success.’
Jen, 44
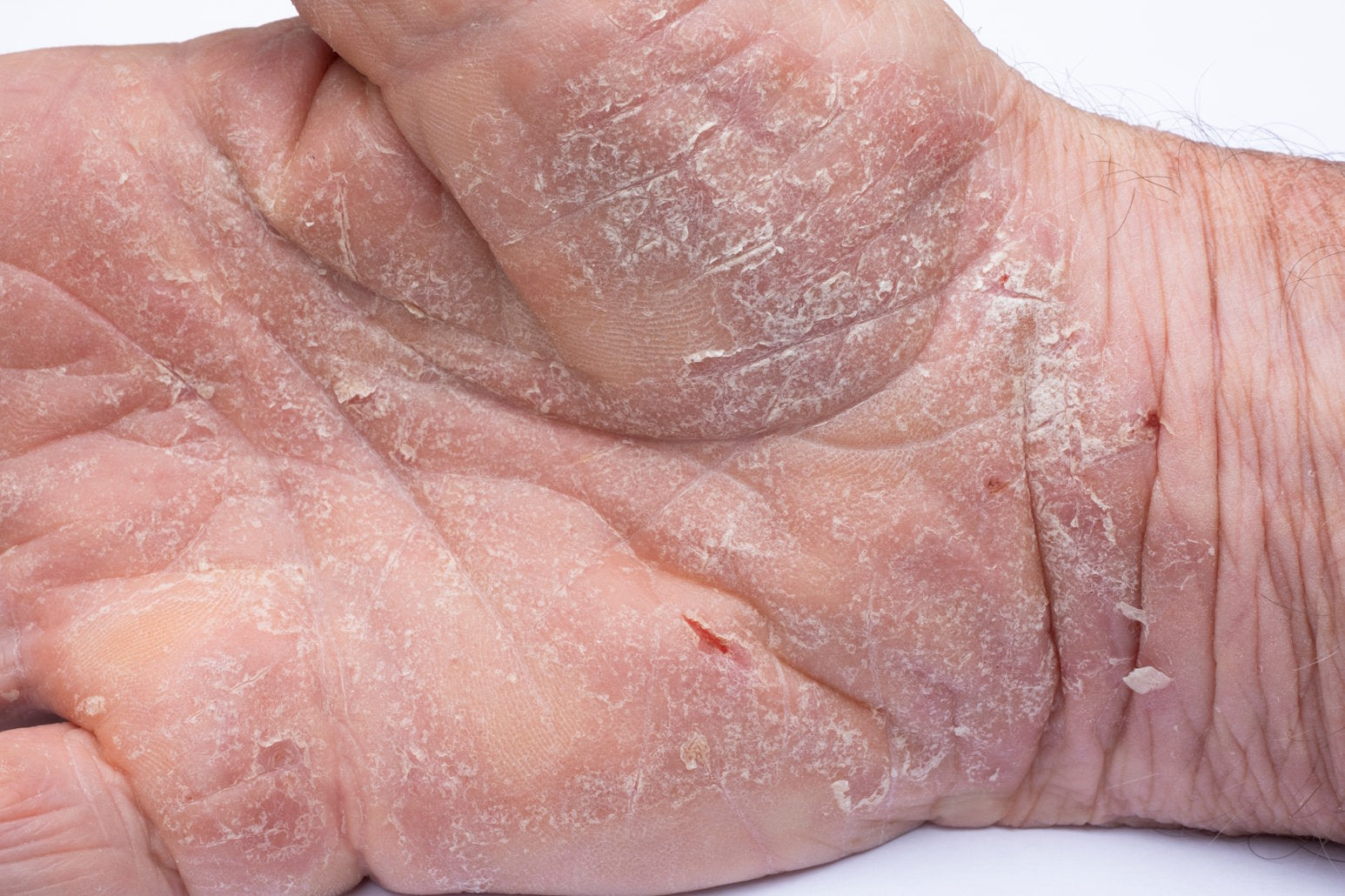
WHAT CAUSES ECZEMA?
The causes of eczema are still not completely understood. Experts do know that people with eczema commonly develop other allergies and that genetic factors can make it more likely for someone to develop eczema. (Source: Allergy.org.au)
The skin barrier of eczema sufferers doesn’t work as well as it does in people without the condition. This is what causes the dry, itchy skin – because the barrier is not working moisture is not retained, so eczema prone skin dries out more easily.
WHAT ARE THE TRIGGERS FOR ECZEMA?
There are many different triggers that can set off an eczema flare up, depending on the type of eczema you have.
Triggers include but are not limited to:
- Artificial colours and preservatives (check out this useful article from ‘eczemalife’ for a list of food additives to avoid)
- Chemicals (like chlorine) found in swimming pools
- Some fabrics such as wool or synthetics like nylon and polyester
- Hot temperatures (living in Australia, it’s hard to escape from those!)
- Stress
- Coming into contact with certain types of carpet or grass
- Bacterial or viral infections
- Scratching
- Dry skin
WHAT ARE THE SYMPTOMS OF ECZEMA?
Everybody experiences different symptoms, but itching is the one thing that most eczema sufferers share in common.
For some people the itch is only mild or moderate and it can be soothed with topical creams. For others the itch gets so bad that the skin becomes inflamed and ends up bleeding from all the scratching (Source: National Eczema Association). It’s just so tough not to scratch when your skin is so itchy you want to peel it all off. We get it!
Other symptoms of eczema, as identified by the National Eczema Association include:
- Dry, sensitive skin
- Darkened patches of skin
- Oozing or crusting
- Swollen areas of skin
- Rough, leather or scaly patches
- Red, inflamed skin
Because there are so many other skin conditions that can cause similar symptoms, it’s a good idea to visit your doctor or dermatologist in order to get a proper diagnosis for eczema. They will be able to recommend the best course of action for your specific symptoms.
TYPES OF ECZEMA
Eczema is actually a general name for a group of eight different conditions. Each of these conditions causes the skin to become red, itchy and inflamed, but may manifest in slightly different ways (Source: National Eczema Association).
It’s helpful to know exactly which type of eczema you have as treatments may vary depending on your symptoms.
The eight different types of eczema are as follows:
Atopic dermatitis
Atopic dermatitis most often starts before age five and may persist through to adolescence and adulthood. It’s more likely to affect people who have a family history of the condition.
The main symptom is a red rash, which most often appears behind the knees or on the arms.
Contact dermatitis
Contact dermatitis is also known as allergic dermatitis. As the name suggests, coming into contact with an allergen sets it off.
The allergen causes a weeping, itchy rash on the contact area, which develops a couple of days after contact and can last for a couple of weeks afterwards.
Did you know that nickel is the most common allergen for contact dermatitis? Nickel can be found in some watchstraps, bra clips, metal clothing studs and costume jewellery. Other causes include plants, chemicals, creams and ointments.
Find out more about the link between nickel and contact dermatitis on the NCBI website.
Australian plants that can cause contact dermatitis include chrysanthemums, primula, tomato plants, grevillea, English ivy and rhus trees (Source:Allergy.org.au). Some vegetables like parsnip or celery can also cause a flare-up. I had a friend who picked parsnips on a farm during her gap year and she developed a nasty case of contact dermatitis on her arms that left her with welts after she also got sunburned!
Dyshidrotic eczema
In this form of eczema, blisters appear on the soles of your feet or palms of your hands. I have this form of eczema and the itching drives me insane.
The tiny blisters are filled with fluid and can last anywhere from two to four weeks. The exact cause is unknown, but experts suggest it could be caused by seasonal allergies or stress.
Hand eczema
Hand eczema is also known as hand dermatitis. Like other forms of eczema, experts believe genetics, allergens or irritants to be the cause.
The symptoms of hand eczema are slightly different to other types of eczema as they include pain, dryness that causes flaking or peeling, cracks, and blisters.
People who work in professions such as hairdressing, cleaning or catering are often affected by this condition due to exposure to chemicals.
Lichen simplex chronicus (LCS)
LCS is an area of chronic eczema and is also known as neurodermatitis. It most often appears on the back of the scalp, neck, lower legs, genitals, wrist or forearms.
The cause of LCS is not full understood. However, it seems to develop after repetitive scratching and rubbing of a localised itch caused by conditions such as psoriasis, insect bites, other types of eczema and lichen planus.
Visit the DermNet New Zealand website for images of LCS and more information.
Numular eczema
This type of eczema looks quite different to other types as it appears as round spots. The spots can be dry and scaly, but can also become open and wet.
Triggers can include:
- Reaction to an inflammation
- Dry skin
- Reaction to metals such as nickel
- Certain medications topical antibiotic creams
- Skin damage from insect bites, scratches or chemicals
(Source: National Eczema Association)
Seborrheic dermatitis
Seborrheic dermatitis mainly affects the scalp, causing scaly patches, red skin and dandruff. In babies it’s known as cradle cap. It can also affect areas such as the face, sides of the nose, chest, eyelids and other oil-prone areas.
Doctors haven’t yet confirmed the exact cause of this condition, however they believe it could be triggered by a yeast called malassezia that is found in the skin’s oily secretions or by an immune system response. (Source: Mayoclinic)
Managing this condition usually involves managing the build up of oils through daily cleansing of the affected areas.
Venous eczema
This type of eczema, also known as stasis dermatitis, is generally caused by circulation problems. People with high blood pressure, kidney failure, obesity, blood clots and congestive heart failure are among those at a higher risk.
It’s generally confined to the lower limbs and is often seen in areas affected by varicose veins. Symptoms include swelling, redness, discoloured skin, scaling, varicose veins and aching legs.
Find out more about the condition and specific treatments at the Dermnet New Zealand website.
WHAT ARE THE BEST TREATMENTS FOR ECZEMA?
Unfortunately there is no cure for eczema, but there are plenty of treatments that can reduce its severity and control flare-ups.
Treatments include:
- Over the counter remedies such as creams and lotions
- Topical medications
- Phototherapy
- Immunosuppressants
- Biologic drugs
- Natural/ alternative treatments
The best treatment for you will depend on your symptoms and the type of eczema you are experiencing. A medical professional should be able to recommend the best treatment regime to help you.
ECZEMA AND ‘LEAKY GUT’
Have you heard about the link between eczema and something called ‘leaky gut’? Some people believe that their eczema is set off by an inflammatory response to a leaky gut, where things like toxins and undigested food particles can escape through the lining of your stomach and into your body via your bloodstream.
Our founder Kiri believes that her eczema was triggered by this condition. This is why she believes in taking an holistic approach to skin care, where diet and lifestyle factors that affect the inside of your body are as important as the products that you use to manage your skin from the outside.
You can read about the science behind leaky gut and inflammatory reactions in this article on the National Eczema Association website.
Find out more about it and how one Australian woman claims to have healed her eczema in this video from YouTuber ‘Cultivate Beauty’.