If you suffer from perioral dermatitis, you will want to understand the treatment options available to help your condition. The best place to start is trying to identify the cause and being aware that there could be several factors at play. While some suggest that demodex mites can cause perioral dermatitis, research indicates this is a secondary phenomenon typically linked to the overuse of topical steroids.
In this article, we share ideas on what the cause of your PD could be and what you can do to help it.

What is Perioral Dermatitis?
Whilst you have no doubt heard of dermatitis, you may not have heard of perioral dermatitis (until you suffer the condition).
Dermatitis is the term given to skin irritation. It is a common condition and can occur in a number of forms including eczema and contact dermatitis. Symptoms are itchy dry skin, rash or swollen, reddened skin. The sufferer may experience skin that blisters, oozes, crusts or flakes off.
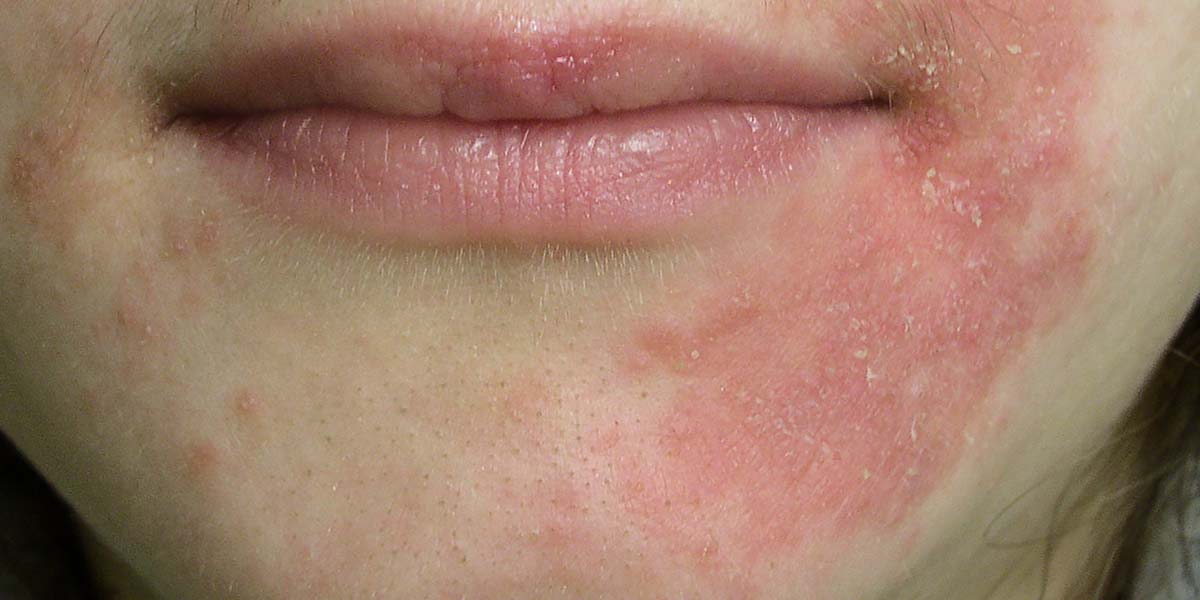
Perioral dermatitis is an inflammatory rash occurring around the mouth, nose, chin and eyes. The name literally means peri (around) oral (the mouth). The rash is made up of small bumps and according to the American Academy of Dermatology (AAD), is usually red in people with light skin and flesh-coloured in people of colour. It typically causes dry, flaky skin, and may involve itching, hence why it is often confused with eczema.
It is significantly more common in women than in men.
Is perioral dermatitis a fungus? Not strictly no, however if you're wondering if perioral dermatitis and gut health are related, it has be linked to an overgrowth of candida in the gut. Poor gut health can manifest on your face in the form of perioral dermatitis. An overgrowth of bacteria in the gut, also known as small intestinal bacterial overgrowth (SIBO), has been linked to both acne and rosacea as well. Experts have performed research into the gut health and the gut microbiome and found links to irregularities in the gut micriobiota before manifestations of dermatitis.
Periocular dermatitis is a form of dermatitis that occurs around the eyes. Some people refer to it as perioral dermatitis of the eyes, and in some cases, it may be confused with or linked to demodex eczema.
What Causes Perioral Dermatitis?
For this condition to develop, several triggers may be to blame:
- It often starts as the ‘side effect’ when topical steroid medication is prescribed for an unrelated rash or skin irritation such as pustular acne. If the medication is used too frequently or misused then stopped, topical steroid addiction/withdrawal can occur. This is sometimes referred to as ‘red skin syndrome’.
- The use of antifungal creams on the face.
- The use of cosmeceuticals including face creams, toners and scrubs.
- Other initiating factors include corticosteroid eye drops, nasal sprays or “preventer” asthma inhalers.
- Allergies to Fluoride, Sodium Lauryl Sulfate (SLS) and Sodium Lauryl Ether Sulfate (SLES)

Are Mites to Blame?
There are medical and non-medical publications stating that increased number of Demodex mites have been observed in perioral dermatitis. The only way to know for sure is through a skin biopsy or scrape at a dermatologist. You might be hard-pressed trying to find a dermatologist willing to perform this though as mites burrow deep into your pores so the results can show as not conclusive.
Demodex is a genus of tiny parasitic mites that live in or near hair follicles of mammals feeding on dead skin cells. They are among the smallest of arthropods with two species Demodex folliculorum and Demodex brevis typically found on humans. Infestation with Demodex is common; prevalence in healthy adults vary between 23-100%. Occasionally some skin diseases can be caused by imbalance in the immune system.
A team at the Department of Dermatovenereology, University Medical Centre Slovenia, were not satisfied that the role of Demodex folliculorum in perioral dermatitis had been satisfactory explained. They tested patients who had previously received topical steroids against those that had not.
Topical steroid addiction/withdrawal can occur when frequently using or misusing moderate to high potency corticosteroids then stopping.
The result was patients who received previous topical steroid therapy had a significantly higher mite density than the patients who had received no topical steroids (p<0.001). Mite density increased significantly with the length of treatment with topical steroids (p<0.001). In conclusion, they suggest that increased density of Demodex folliculorum in perioral dermatitis is a secondary phenomenon, associated with topical steroid therapy. You can read about the study here: https://www.ncbi.nlm.nih.gov/pubmed/16040404
The best way to know if mites are to blame is to look at the pattern of your rash and how well you respond to the treatment for Demodex. Often when treating Demodex you might see problems move to other areas of your face because the mites will actually escape the area that you’re treating, so that’s a really important clue.
Also, if you have rash around your eyes or eyebrows that’s another indication that it’s likely mites since they tend to gravitate towards naturally hairier areas of the face.
Demodex mites will rarely live inside your mouth as they eat cells that line hair follicles.

What Helps Get Rid of Perioral Dermatitis?
To clear up your perioral dermatitis, there are a few actions to take:
You should stop using corticosteroids, including hydrocortisone cream
The American Academy of Dermatology (AAD) recommends ceasing topical steroids but cautions the rash can worsen before it gets better (this is known as steroid withdrawal). If you have been using topical steroids for a prolonged period of time you should not stop using suddenly, and should instead slowly wean off them under the supervision of a medical professional.
Change your skin care routine
The AAD also recommend you should focus on your skin care routine. “Skin care can play an important role in treating this rash. You may need to switch to a mild, fragrance-free cleanser and be very gentle when you wash your face. You may need to use fragrance-free skin care products.”
Use active “good bacteria” products
The skin has billions of microflora (made up of both good and bad bacteria) living on its surface. This is what’s referred to as our ‘microbiome’. When these bacteria are out of balance, they can contribute to chronic skin problems. This is where probiotics can help.
Probiotics are the good bacteria and yeasts that provide benefits for the overall health of our digestive system. These microorganisms have the capacity to balance bacteria in the gut and to block pathogens.
Topical versions can play a beneficial role, soothing inflammation, having a calming effect and gently repairing the skin. In short, probiotics are good for perioral dermatitis.
The hero ingredient in the AMPERNA® range is the active probiotic complex, Lactococcus ferment lysate. This probiotic complex helps support the skin barrier; helping to protect you from aggressors such as environmental pollutants, helps keep your immune system in check and helps reduce inflammation.
In short, it acts as a protective layer on the skin, helps boost healthy looking skin and helps calm & soothe skin.
Does apple cider vinegar help perioral dermatitis?
Whilst some natural ingredients are beneficial to the skin, some have no value whilst others can cause problems. The issue with ACV is it is a harsh solution that can remove your skins protective layer, remove moisture from your skin, and cause it to become more irritated. There are also other ingredients to avoid with perioral dermatitis such as SLS, SLES and fluoride.
What bacteria causes perioral dermatitis?
The truth is that you have good and bad bacteria all over your skin all the time. Balanced skin is happy skin. So if you have a compromised skin barrier; you may have more bad bacteria on your skin, which in turn may lead to irritation and perioral dermatitis.
AMPERNA® is in fact the first Australian brand to bring you a full range of probiotic skincare products, for even the most sensitive skin or that you can tailor to any skin concern, and the first to use this particular probiotic strain in any Australian skincare product.
If you are experiencing a perioral dermatitis flare, you can wash with water and the gentle Soothing Duo.
How Long Will it take to Get Rid of Perioral Dermatitis?
The short answer is it depends on what the cause is. It may take a few weeks or up to a few months to clear completely and everyone's journey will be different.
Kiri, founder of AMPERNA® will work with you to implement a holistic regime to help your condition.
Sources:
https://www.aad.org/public/diseases/rashes/perioral-dermatitis
https://www.dermcoll.edu.au/atoz/perioral-dermatitis/
https://www.ncbi.nlm.nih.gov/pubmed/16040404